Introduction to ortho-perio interrelationship
Orthodontic treatment has become one of the most commonly carried out dental treatment in adolescents and young adults. The most commonly argued rationale for this treatment is that dental alignment obtained with orthodontic therapy facilitates plaque removal and reduces occlusal trauma. The bristles of the toothbrush fail to reach all tooth surfaces when the teeth are severely crowded. After orthodontic treatment, once the proper alignment of teeth is achieved, plaque removal by self-performed plaque control measures become easy which contributes to a good periodontal health. The success of orthodontic treatment depends on the patient’s periodontal status before, during and after active treatment. The most commonly encountered problems in patients with compromised periodontal status are migration, extrusion or flaring of teeth that may occur if improper orthodontic forces are applied. If orthodontic treatment has to be carried out in a periodontally compromised patient, an interdisciplinary approach is followed in establishing a comprehensive treatment plan for the patient.
Objectives of orthodontic tooth movement in periodontally compromised patients
The prime requirement of orthodontic treatment is healthy and sound periodontium. If periodontal health is compromised, orthodontic treatment becomes difficult. Hence, a multidisciplinary approach is required to treat these complex conditions. An appropriately done orthodontic treatment in periodontally compromised patients should achieve following goals,
- It allows better maintenance of oral hygiene by the patient, thus reducing the chances of periodontal disease progression.
- It results in occlusal contacts which are able to appropriately transfer occlusal forces to the alveolar bone.
- It contributes, along with prosthetic rehabilitation, to a normal vertical dimension.
- In selected cases, orthodontic treatment results in the establishment of an appropriate crown-root ratio, resulting from extrusion or intrusion.
- Orthodontic treatment may facilitate improved bone support in areas with the vertical bone loss.
- It improves the position and angulation of the abutment to better support fixed prosthodontic prosthesis.
- A properly aligned arch form results in better maintenance of dental and periodontal health for a long duration of time.
Can orthodontic treatment help in the prevention of periodontal disease progression?
It has been well established that abnormal positions of the teeth in the dental arch is a predisposing factor for periodontal disease progression 1, 2. A significant correlation has been found between malocclusions and periodontal condition, suggesting malocclusions as risk markers for periodontal diseases 3. The accumulation of periodontal pathogens in anterior areas with crowded teeth has been shown to be much greater than non-crowded sites 4. Orthodontic treatment also helps in the elimination of occlusal abnormalities, thus preventing periodontal tissue damage due to abnormal occlusal forces 5. In one study, Brown (1973) 6 investigated the effect of molar uprighting on its periodontal health. Seven months following the treatment it was found that there was 2.5 mm greater ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
Periobasics: A Textbook of Periodontics and Implantology
The book is usually delivered within one week anywhere in India and within three weeks anywhere throughout the world.
India Users:
International Users:
Studies have been done to analyze the effect of extrusion on periodontal health. Ingber (1974, 1976) 8, 9 demonstrated that some probing depth can be achieved after tooth extrusion. The beneficial effect of forced tooth extrusion to facilitate prosthetic treatment in healthy periodontium has also been demonstrated 10. Similarly, studies have been done to analyze the effect of intrusion on the periodontium. It was shown in one study that intrusion is best performed under light orthodontic forces (5-15 g/tooth) in the presence of gingival health 11.
It must be noted that adequate plaque control and gingival health are primary requisites for orthodontic treatment. It has been demonstrated in animal studies that in the absence of adequate plaque control, orthodontic forces can cause angular bone defects and if the intrusion is attempted, attachment loss can occur 12. Many animal ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
Two systematic reviews were published by Bollen to find out the answer to the following question: does a malocclusion affect periodontal health, and does orthodontic treatment affect periodontal health? The results from the first review (2008) 18 revealed that there was a positive correlation between the presence of a malocclusion and periodontal disease. Patients with greater malocclusion had adverse periodontal status as compared to patients ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
Cellular and molecular biology of orthodontic tooth movement
A large variety of cells and molecular factors are involved in bone remodeling during orthodontic tooth movement. Let us first discuss the molecular factors which are involved in initiating extracellular matrix changes and cellular mobilization following the application of orthodontic forces.
Molecules involved in bone remodeling during orthodontic movement
Orthodontic forces result in areas of pressure and tension around teeth which initiate the local inflammatory reaction. This reaction is mediated by various mediators which act on their target cells. The most important of these mediators are cytokines, growth factors, and transcription factors.
Cytokines:
Cytokines are important signaling molecules responsible for various biological actions. They act on nearby cells in an autocrine or paracrine fashion to facilitate cell to cell communication. The cytokines involved in bone metabolism include interleukin 1 (IL-1), tumor necrosis factor-α (TNF-α), interleukin 2 (IL-2) interleukin 3 (IL-3), interleukin 6 (IL-6), interleukin 8 (IL-8), gamma interferon (IFN-γ), and osteoclast differentiation factor (ODF). Out of these cytokines, IL-1β and TNF-α have been shown to be potent stimulators of bone resorption 20, 21. IL-1 stimulates bone resorption by stimulating osteoclastic function through IL-1 type 1 receptor, expressed by osteoclasts. IL-1 acts as a strong chemoattractant for leukocytes and stimulates fibroblasts, endothelial cells, osteoclasts, and osteoblasts. On the other hand, TNF-α can directly stimulate the differentiation of osteoclast progenitors to osteoclasts in the presence of macrophage colony-stimulating factor (M-CSF). The expression of both IL-1 and TNF-α has been found to be increased ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
Another important cell signaling system involved in bone remodeling is RANKL/RANK/OPG system 23. The TNF-related ligand RANKL (receptor activator of nuclear factor-Kappa ligand) and its 2 receptors, RANK and osteoprotegerin (OPG) play a vital role in bone remodeling. A detailed description of RANKL/RANK/OPG system has been given in chapter 11 “Osteoimmunology in periodontal health and disease”.
Growth factors:
Growth factors play a vital role during bone remodeling. Growth factors found to play a vital role during bone remodeling are fibroblast growth factor (FGF), epidermal growth factor (EGF), platelet-derived growth factor (PDGF), transforming growth factor-β (TGF-β), insulin growth factor (IGF), bone morphogenetic proteins and connective tissue growth factor (CTGF). Transforming growth factor-beta (TGF-β) family includes TGF-β1, activins, inhibins, and bone morphogenetic protein which play a vital role in bone metabolism. The functions of FGF and IGF are almost similar 24. They act on fibroblasts, endothelial cells, myoblasts, chondrocytes, and osteoblasts. PDGF is secreted by platelets which migrate from the blood vessels to the extravascular space because of inflammation resulting from orthodontic forces 25. CTGF protein is associated with the ECM remodeling during anabolic bone remodeling 26. It stimulates proliferation of osteoblast precursors and promotes mineralization of new bone by osteoblasts. A detailed description of growth factors and their functions has been given in “Application of growth factors in periodontal regeneration”.
Role of transcription factors:
The non-collagenous bone matrix proteins include osteopontin, bone sialoproteins, osteocalcin, and osteonectin. These proteins play an important role in initial mineralization of bone. It has been found that Runx2 (Cbfa1) and osterix (Osx) transcription factors are required for the expression of ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
Extracellular remodeling during orthodontic tooth movement
The periodontium supporting and investing the teeth consists of periodontal ligament (PDL), alveolar bone, cementum, and gingiva. Periodontal tissues are constantly subjected to remodeling to adapt to the changes in environmental conditions. Various cells involved in periodontal remodeling include fibroblasts, osteoblasts, osteocytes, osteoclasts, odontoblasts, cementoblasts, chondrocytes and immune cells. The major cells found in PDL are fibroblasts 29-31. PDL plays a very important role during orthodontic tooth movement. It is primarily made up of Type I and Type III collagen fibers with predominantly Type I fibers 32, 33. Elasticity to PDL is provided by ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
When orthodontic forces are applied on teeth, these cause biophysical and biochemical changes in the extracellular matrix of PDL and also effect constituent cells of the periodontium and dental pulp 35-38. Due to orthodontic forces, areas of pressure and tension are created in the PDL which cause fluid displacement in the extracellular matrix of PDL. This fluid displacement causes physiological activation of PDL fibroblasts, osteocytes, osteoblasts, bone lining cells and osteoblasts/osteoprogenitor cells 39. The nociceptive stimulus causes PDL fibers associated neurons to release neuropeptides such as Substance P, calcitonin gene-related peptide 40-43. Under the influence of these peptides as well as PGE2 and other humoral factors capillary dilatation in PDL occurs, resulting in the release of immune-competent cells from the capillaries 37. The migration of these cells from capillaries to extracellular matrix (ECM) is facilitated by vascular endothelial growth factor (VEGF), secreted by endothelial cells and osteoblasts.
Various changes in the ECM and cellular re-organization initiate the remodeling process. Phosphorylation of cellular proteins including extracellular signal-regulated kinases (ERK) occurs because of changes in the cytoskeleton, which triggers signal transduction via integrins/ fibronectin/ kinase- pathway 44-46. The matrix metalloproteinase (MMP) are involved in connective tissue remodeling by their action of degradation of matrix components. These matrix degrading enzymes increase in pressure areas around the tooth subjected to orthodontic forces. Particularly, MMP- 1, 8, 9, 3, 13 are increased in these sites. Along with this, Prostaglandin ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
Cellular re-organization during orthodontic treatment
The modifications in the ECM are followed by the cytoskeleton re-organization in osteoblastic cells. This re-organization results in phosphorylation of cellular proteins including extracellular signal-regulated kinases (ERK) 44 which initiate signal transduction via integrins/ fibro-nectin/kinase pathway 46, 50, 51. Prostaglandin production and increase in cyclic ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
The proliferation of new osteoblasts is required for bone remodeling. The formation and proliferation of preosteoblasts requires signaling through the Wnt-frizzled-low density lipoprotein 5 (LRP5 receptor-related protein)-β-catenin signaling pathway 52. It has been shown that deficiency of LRP5 can cause osteoporosis both in mice and humans 53. The mature osteoblasts which are responsible for new bone formation by deposition of the extracellular matrix also require signaling protein ATF4 along with LRP5 54. The present data suggests that osteoblasts lining the bony socket are directly responsive to strain such as orthodontic forces through the ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
Osteocytes are trapped osteoblasts in the bone matrix. The present data suggests that these cells are very proprioceptive 57. It has been shown that mechanical strain within physiological limits causes increased expressions of glucose-6-phosphate dehydrogenase, 3H-urinidine, c-fos, and IGF-I in the osteocytes measured within 6 h after application of intermittent loading at physiological strain magnitude 58.
Osteoclasts or bone-resorbing cells are differentiated from monocyte-hemopoietic cells. These are multinucleated giant cells found in bay-like depressions of bone called Howship’s lacunae. These resorb the bone matrix by dissolving the bone minerals. Active osteoclasts can be identified by their high content of tartrate-resistant acid phosphatase (TRAP).
In the areas of compression, due to inflammatory response, there is the release of pro-inflammatory mediators which lead to increased vascularity. Due to increased vascularity, there is increased capillary blood supply and increased number of cells including osteoclasts and fibroblasts. Under light forces, bone resorption takes place just below the area of pressure on the PDL side (frontal resorption) whereas under heavy pressure, because of excessive compression of PDL, its ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
Cascade of events following application of orthodontic forces
There are three histological events that have been explained on the basis of current knowledge that take place after the application of orthodontic forces. The first event is related to alteration of blood vasculature. As already stated, following the application of orthodontic forces the blood supply is altered both in areas of tension as well as pressure areas. This causes decreased oxygen level at the compressed area and probably increased oxygen level at tension areas 59, 60. The second event is the generation of an electrical signal. Due to bending of bone and deformation of the crystallization structure, a Piezoelectric signal or more appropriately referred to as a bioelectric potential in the form of a small voltage of current is generated 61. Thirdly, the physical distortion imposed by peripheral forces on paradental tissues such as nerve fibers and terminals results in the release of various neurotransmitters such as Substance P, Vasointestinal polypeptide (VIP) and calcitonin gene-related peptide 61.
All these signals result in activation of cells in the periodontal ligament and bone. It has been shown that PDL fibroblasts and bone cells, such as osteoblasts possess receptors for the chemical mediators released after the application of orthodontic forces. Along with this, these cells are highly interactive and interconnected, creating a lot of possibilities of signal transduction 62. Once these signals are received by these cells, it causes a transient increase in the intracellular levels of second messengers including cyclic adenosine monophosphate (cAMP), cyclic guanosine monophosphate (cGMP), inositol phosphatase 3 (IP3) and calcium 63-66. These second messengers then advance these signals to the nucleus by a series of kinases. It results in gene expression in the form of protein transcription factors such as C-fos, C-jun AP-1 mRNA, Egr-1, SP-1 growth ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
Sequence of orthodontic treatment in periodontally compromised patients
A systematically planned approach is designed for the orthodontic treatment in periodontally compromised patients. According to Mathews and Kokich (1997) 70, the orthodontic treatment of a periodontally compromised patient consists of following steps,
Periodontal examination by the orthodontist,
Periodontal screening and recording.
Periodontal probing.
Attached gingiva.
Radiographs.
Parafunction.
Pre-orthodontic periodontal therapy,
Pre-orthodontic osseous surgery,
Osseous craters.
Three-wall intrabony defects.
Hemiseptal defects.
Furcation defects.
Root proximity.
Pre-orthodontic gingival surgery,
Gingival grafting.
Root coverage.
Orthodontic treatment,
Appropriately selected fixed orthodontic appliance.
Constant monitoring of periodontal health.
Post-orthodontic phase,
Retention for more than 6 months.
Definitive restorative and occlusal therapy.
A three-month periodontal maintenance program.
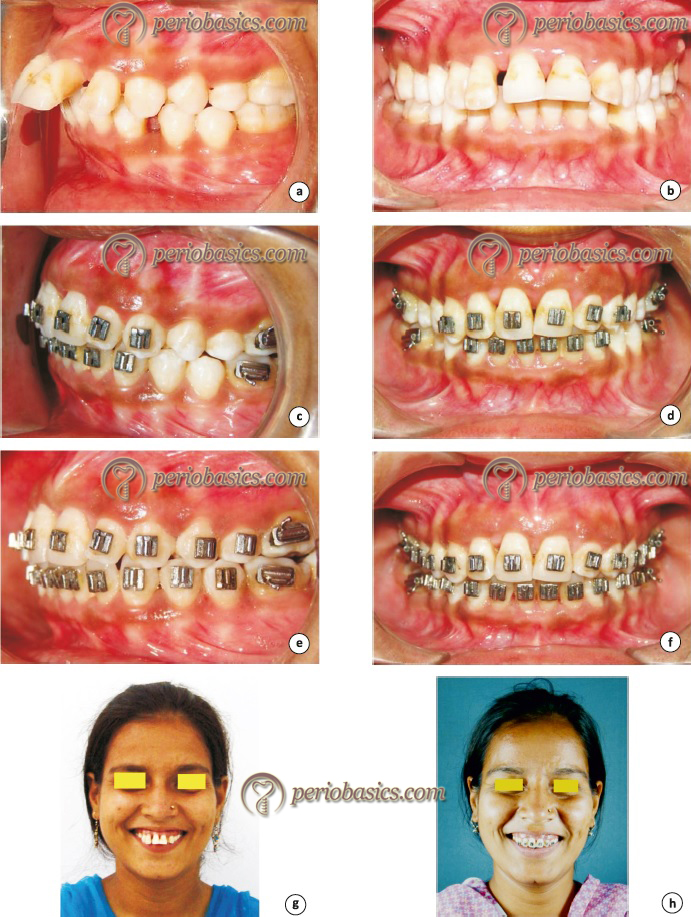
Periodontal examination by the orthodontist
Orthodontist plays a very important role in the identification of periodontal problems, especially in an adult patient undergoing orthodontic treatment. An orthodontist must incorporate compulsory periodontal examination during the initial consultation with the patient. Periodontal screening and recording (PSR) is a simple, quick and effective method of recording the periodontal status of the patient with minimum documentation 71. In this examination, a score is given to each area which helps the examiner to decide what kind of periodontal treatment is required for a particular patient. The width of ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
Radiographic examination is required for the evaluation of the generalized bone topography. Intraoral periapical, panoramic or bitewing radiographs may be advised as required. For evaluation of periodontal osseous lesions, panoramic radiographs are not as suitable as the periapical or bitewing radiographs. The most common areas that are missed in a panoramic radiograph includes interproximal craters between upper molars, infrabony defects on the mesial of the upper first bicuspid, and defects around the lower incisors. The crestal bone is more clearly visible in bitewing radiographs.
Patients who are bruxers or clenchers must be identified during the initial consultation because it has been shown that these parafunctional habits can cause extensive osseous breakdown during orthodontic therapy 4. These patients may need a night guard while undergoing active orthodontic treatment.
Periobasics: A Textbook of Periodontics and Implantology
The book is usually delivered within one week anywhere in India and within three weeks anywhere throughout the world.
India Users:
International Users:
Pre-orthodontic periodontal therapy
The pre-orthodontic periodontal therapy includes the elimination of etiological factors such as plaque, calculus, and occlusal trauma. Along with this, patient is educated about the importance of good oral hygiene during orthodontic treatment and instructed to maintain a good oral hygiene. Root planing and subgingival debridement is done to minimize inflammation. The patient is re-evaluated for the periodontal status and this initial phase of treatment lasts up to 3 months. The periodontist must ensure that the patient is periodontally stable to undergo orthodontic treatment. If some areas require surgical intervention, the surgical periodontal therapy is planned before orthodontic treatment. These surgeries include the following,
Pre-orthodontic osseous surgery
The decision regarding surgical periodontal therapy is taken after evaluation of the patient after non-surgical periodontal therapy. In areas with moderate to deep periodontal pockets, periodontal flap surgeries are planned and regenerative or resective osseous procedures which will facilitate orthodontic tooth movement are done during the surgery. The most common osseous defect encountered is osseous craters. These defects can be eliminated by reshaping the defect and reducing the pocket depth 72, 73. One or two wall defects need special attention because any tooth movement into these defects may reduce the bone support of the tooth leading to increased tooth mobility. These defects are commonly seen on the mesial aspect of mesially tipped teeth and teeth which have supra-erupted. These defects can be eliminated with appropriate orthodontic treatment. Uprighting of the molars and intrusion of supra-erupted teeth usually eliminates the defect if the area is kept free of inflammation 6, 8. The three wall defects can be ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
Furcation lesions need special attention because they are the most difficult lesions to treat. In patients who are planned for orthodontic treatment, these defects may create complications during the treatment. The Grade I defects have a good prognosis and can be treated by osseous surgical correction. The Grade II furcation defects can be treated with grafting and regenerative therapy with barrier membranes. Grade III and Grade IV defects are more difficult to treat. The regenerative procedures may not be very successful in these defects and procedures like hemisection, root amputation or even tooth extraction followed by implant placement can be planned for these defects. More detail regarding management of teeth with furcation involvement is given in “Furcation involvement and its management”. Placement of orthodontic band around ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
Closely placed roots provide areas for plaque accumulation and are difficult to maintain by the patient. Close root proximity between the distobuccal root of the upper first molar and mesiobuccal root of the upper second molar creates a difficult situation to treat surgically without root amputation. With appropriate orthodontic treatment, this problem can be resolved without periodontal surgery by the intrusion of the first molar, bone leveling, and opening up the embrasure space between the first and second molar roots.
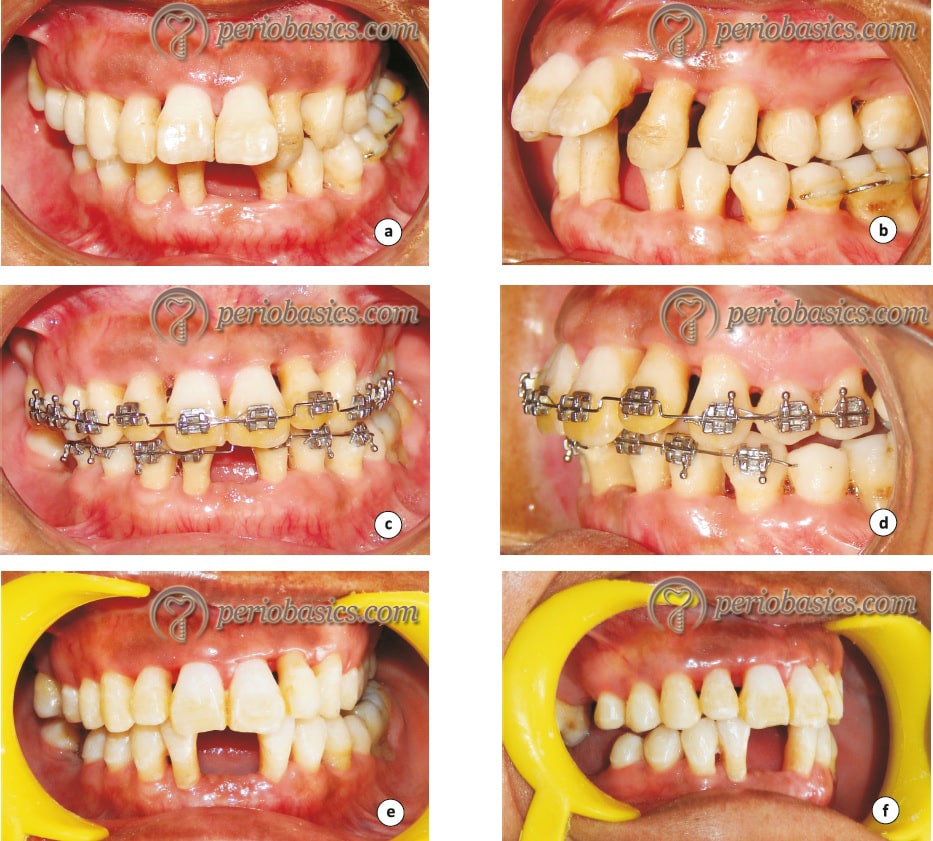
Pre-orthodontic gingival surgery
The gingival surgeries before orthodontic treatment are done to increase the width of attached gingiva or for root coverage or for both the purposes. The areas which have less than 2 mm of attached gingiva should be considered for a free gingival graft procedure to increase the width of attached gingiva. Teeth which have to be proclined orthodontically have more chances of recession and dehiscence. Root coverage procedures are done in areas of recession to cover the exposed root surfaces. If orthodontic treatment has been planned for a patient, root coverage procedures for esthetic purpose should be done after the ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
Orthodontic treatment phase
This phase involves placement of fixed orthodontic appliance selected for an individual patient. The periodontally compromised patient may have different kinds of bone loss patterns and the orthodontic treatment should be planned, keeping in mind the type of bone loss pattern. Following bone loss patterns are commonly seen in periodontally compromised patients going for orthodontic treatment,
Orthodontic treatment in patients with horizontal bone loss:
In a periodontally healthy individual, the placement of brackets is primarily determined by the incisal edges in the anterior teeth and by marginal ridges in the posterior teeth. However, in patients with a significant horizontal bone loss, the scenario for bracket placement changes. Here, considering the crown anatomy for bracket placement is inappropriate. Because the bone level may recede several millimeters from the cementoenamel junction, the crown root ratio is altered. By aligning the teeth, tooth mobility may increase and significant bony discrepancies may appear between healthy and periodontally diseased roots. In these cases, the orthodontist can use the bone level as a guide to positioning the brackets on the teeth. Tooth equilibration should be done to establish appropriate incisal edge relationship. If the tooth is vital then equilibration should be done gradually to allow the formation of secondary dentin.
In cases of advanced horizontal bone loss, teeth should be evaluated for their long-term prognosis. If a tooth has a good prognosis, it should be retained and if indicated surgical therapy should be done to further improve its prognosis. Following the surgical periodontal therapy, a period of 6 months should be given for the stabilization of the periodontal condition of the patient before the orthodontic treatment is started.
Orthodontic treatment in patients with hemiseptal defects:
Hemiseptal defects are one- or two-wall osseous defects that are often found around mesially tipped teeth or super-erupted teeth. In periodontally healthy patient, the brackets are placed on posterior teeth, according to marginal ridges and cusps. However, some adult patients may have marginal ridge discrepancies caused by uneven tooth eruption. In these patients, the bracket placement is not solely determined by the anatomy of the tooth but also by assessing the teeth radiographically to determine the interproximal bone level.
If the bone level is oriented in the same direction as the marginal ridge discrepancy, bone leveling can be easily done by leveling the marginal ridges. On the other hand, if the interdental bone level is flat and the marginal ridges are at significantly different levels, leveling of marginal ridges discrepancy orthodontically will produce a hemiseptal defect in the bone. This may result in the formation of a periodontal pocket between the two teeth.
In some cases, the discrepancy between both the marginal ridges as well as the bony levels between two teeth may exist. Also, these discrepancies may be of different magnitude. In such cases, orthodontic leveling alone may not be able to eliminate the discrepancy in the marginal ridges. So, the crowns of the teeth should ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
When teeth are extruded to level the hemiseptal defect, the patient should be kept under constant observation. The sulcus depth is more initially and is difficult to clean, but as the defect ameliorates with extrusion of the tooth, interproximal cleaning becomes easy. The re-evaluation of the patient should be done every 2-3 months.
Furcation defects:
As already stated, for Grade I and Grade II furcation involvement regenerative therapy is the treatment of choice and has been shown to provide good results. However, Grade III furcation defects may not produce consistently satisfactory results. These cases may be treated by hemisection of the tooth or removal of the involved root. A detailed information regarding the treatment of teeth with furcation involvement is available in the “Furcation involvement and its management”.
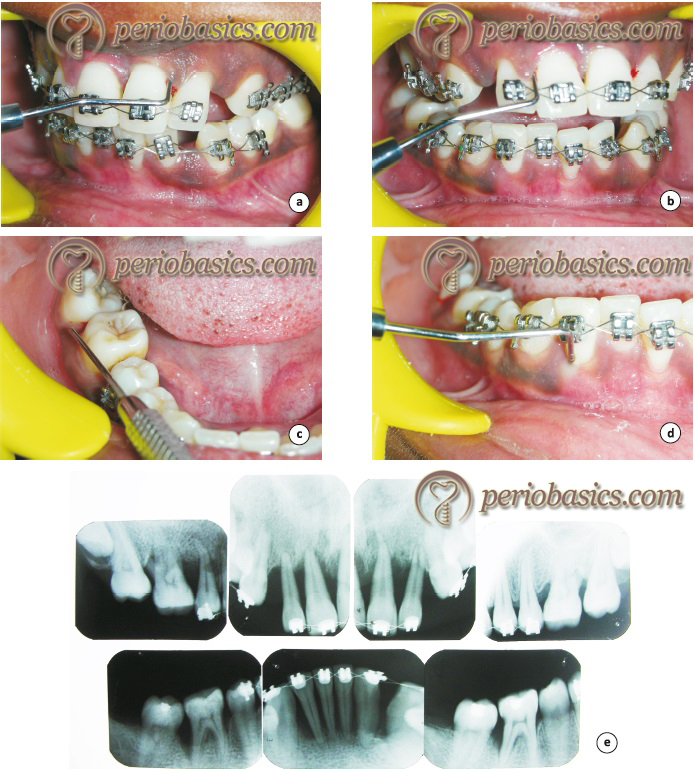
Various tooth movements in various conditions in periodontally compromised patients
During orthodontic treatment in periodontally compromised case, the prime objective is to make sure that there is minimal inflammation in the periodontal tissues and the orthodontic forced are light enough not to cause deleterious hydrostatic pressure in the periodontal ligament 75, potentially increasing the risk of root resorption 76. Commonly, patients with compromised periodontal status are adults who had an active periodontal disease which has resulted in present periodontal status. It should be noted that with increasing age, periodontal tissues become richer in collagen and its blood supply is diminished. As a result of this, the periodontal response to orthodontic forces commonly results in the establishment of hyalinization zones 77. When hyalinization zones are formed, tooth movement is hampered and a complex reparative process is installed. Tooth movement occurs only after the ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
Labial tooth movement/proclination:
These tooth movements are very commonly done orthodontic movements to resolve crowding. However, proclination may result in recession, especially in lower anterior teeth 79. A common reason for recession in these areas is the minimal thickness of soft tissue and bone covering the root surfaces 80. Hence, the tissue biotype, as well as the thickness of the alveolar bone over the root surface, should be evaluated before subjecting it to labial forces so that mucogingival problems can be avoided.
Molar uprighting:
Molar uprighting is usually considered for mesially tipped molars. It usually results in improvement in pocket probing depth and in the crown-root ratio 6. However, if the molar has furcation involvement, the up-righting ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
One major problem associated with molar uprighting is furcation involvement. It has been observed that furcation defect remains the same or gets worsened following up-righting of molars. This is because along with up-righting there may be some degree of extrusion also which increases the severity of furcation involvement. The severity of involvement is further increased if inflammation is present 81. One suggested treatment for molars with furcation involvement is splitting the two roots and keeping one or both the roots which are then orthodontically moved into new positions. However, this treatment is difficult and requires close observation during orthodontic tooth movement 82. There are conflicting results regarding the effects of molar uprighting on its periodontal support. According to Lang (1977) 83, molar uprighting is a predictable procedure if excellent oral hygiene is maintained. On the other hand, Kessler (1976) 84 has reported that orthodontic molar uprighting may result in a greater degree of furcation involvement and tooth mobility.
Orthodontic extrusion and intrusion:
It is well established that gingival tissues significantly follow dental movements 85. Orthodontic extrusion was initially used for increasing the length of clinical crown and/or to change the height of the free gingival margin 85, 86. Further, extrusion also results in re-establishment of crestal bone level because the relationship between cementoenamel junction and its bone crests is roughly maintained. In one study 14, forced extrusion was done for maxillary incisors in monkeys. It was concluded that if appropriate oral hygiene is maintained, the sulcus depth is maintained with no periodontal pocket formation or significant inflammation. The attached gingiva moves approximately 80% of the vertical tooth movement with minimal changes in the mucogingival junction. However, the risk of relapse is there, so fixed permanent or semi-permanent retainers are recommended in these cases. Experimental studies have demonstrated that the recession during orthodontic extrusion is not due to tooth movement, but due to poor hygiene control of the associated teeth 13, 15, 87-91.
Studies have been done to evaluate the extrusion with and without fibrotomy of the supracrestal attachment gingival fibers. It has been observed that forced extrusion without supracrestal fibrotomy results in bone remodeling with the increase of the width of the attached gingiva, crestal bone deposition, and some gingival margin recession. On the other hand, with supracrestal fibrotomy, extrusion was significantly greater along with gingival recession and attachment ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
The orthodontic intrusion may be indicated in cases where teeth have suffered horizontal loss or are supra-erupted due to lack of the antagonist tooth. Maintenance of adequate oral hygiene during forced intrusion is essential because the presence of plaque biofilm around the gingival margins around the tooth may facilitate ingress of plaque into the subgingival area during the intrusion, provoking or aggravating the ongoing process of periodontal destruction 13-15, 98. The gingival position partially follows induced orthodontic intrusion 84, 99, 100. In one study, where orthodontic intrusion was done for lower incisors in patients with an intact periodontium, the apical movement of gingival margin and the mucogingival junction was found to be 79% and 62%, respectively 101. For orthodontic intrusion in periodontally compromised cases, the available data suggests that there is a significant ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
Orthodontic correction of trauma from occlusion (“jiggling” forces):
One of the major objectives of clinical orthodontic practice is to correct occlusion disorders. It is well established that inappropriate occlusal forces can cause bone loss and attachment loss in healthy periodontium 4, 104. Adjustment of these occlusal abnormalities is mandatory to ensure a good periodontal health of involved tooth/teeth. Occlusal trauma in one or more teeth may be associated with parafunctional responses such as clenching and bruxism. However, lack of established criteria to determine the severity of occlusal trauma is a problem for delivering occlusal treatment. The diagnosis of trauma from occlusion is made on the basis of clinical and radiographic findings, including increased tooth mobility, unfavorable crown root ratio, widening of PDL space and vertical bone loss around involved tooth. Presently, there is insufficient evidence to clarify the extent to ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
After the completion of orthodontic treatment, it is important to analyze occlusion. A correct cusp-fossa relationship cannot always be achieved after orthodontic treatment. So, occlusal adjustments may be required following orthodontic treatment. A stable occlusion after orthodontic treatment should have following features 105,
- Stable tooth contacts in centric occlusion.
- A straight forward slide from centric relation to centric occlusion without any lateral deviation.
- Smooth gliding contacts in centric and eccentric mandibular motion.
- No balancing side interferences.
Elimination of occlusal abnormalities with orthodontic treatment may favor healing of periodontal defects, especially the infra-bony defects after periodontal treatment. Further, a properly aligned dentition with a stable occlusion is a good prognostic factor for long-term periodontal maintenance of the patient.
Correction of missing interdental papilla:
In advanced periodontal destruction, loss of interdental papilla is a common finding. The esthetic improvement in such cases usually requires a combination of enameloplasty (inter-proximal reduction), tooth movement and selective addition of composite resin. If by performing only orthodontic tooth movements clinically acceptable results cannot be achieved, the direct-bonding resin can be added to lower the contact point and create the illusion of a healthier papilla 106. However, such treatments require a thorough knowledge of facial esthetics.
Correction of gummy smile:
There are many reasons for a gummy smile which may be related to the growth pattern of the maxilla, retardation of the physiological apical migration of gingival margins with thick gingival phenotype or extrusion of maxillary anterior teeth (Angle class II, division 2 malocclusions). The cause of gummy smile has to be analyzed first and accordingly, treatment is ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
Periodontal regenerative therapy and orthodontic treatment
In the advanced periodontal bone loss, various regenerative procedures such as guided tissue regeneration (GTR) with or without bone graft are attempted wherever indicated. GTR with the osseous grafting procedure is most documented for histological evidence of periodontal regeneration 107, 108. The impact of the regenerative procedure on orthodontic tooth movement and ideal timing for orthodontic tooth movement following regenerative therapy have been a field of extensive research. Experimental studies on dogs with Grade II furcation lesions have demonstrated that 60 days delay in orthodontic treatment did not interfere with healing or adversely impact the amount of bone regeneration by regenerative periodontal techniques 109-112. However, it must be remembered that the bone remodeling cycle (sigma) is 3 months in dogs and 4.25 months in humans 113. Hence, healing in humans to a comparable level is likely to take a longer time.
Many clinical investigations have demonstrated that following treatment with GTR with osseous grafting, orthodontic tooth movement does not cause any adverse effect on periodontal tissue support 114-117. However, a clinical review found a low level of evidence that teeth moved successfully into the grafted area with various types of bone grafts (non-autogenous) and there were no deleterious effects on the roots of teeth 118. Studies on dog models have shown that following regenerative therapy with GTR procedure, orthodontic tooth movement can be started as early as 60 days following the GTR procedure 109. This time interval was thought to be required for appropriate periodontal healing and to prevent orthodontic tooth movement from interfering with the healing process.
In a recent prospective clinical trial, the effectiveness of different times of initiating the active orthodontic tooth movement on the regenerative potential of the intrabony defects was evaluated. The results of the study demonstrated that one year after GTR procedure, better results were obtained in a group of patients where orthodontic tooth movement was initiated immediately after the bone grafting procedure as compared to subjects in which tooth movement was ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
The present evidence suggests that in a healthy periodontal environment, orthodontic tooth movement does not adversely affect the results obtained from regenerative procedures. However, whether to delay tooth movement after the regenerative procedure or not is still a matter of research and most of the clinicians prefer to wait for 4 to 6 months following all kinds of active periodontal treatments.
Clinical situations where orthodontic treatment should be avoided
1. Uncontrolled infection and inflammation.
2. Lack of retention for stabilization of teeth in their new position.
3. Inadequate space into which teeth can be moved.
4. Movement of teeth against occlusal opposition or into occlusal trauma.
5. Movement of teeth in conditions where periodontal health, function or esthetics will not improve.
6. Movement of teeth against inadequate anchorage.
7. Movement of teeth into unfavorable environment.
8. Lack of patient motivation and cooperation.
9. Tooth movement in patients with systemic problems that cannot be treated or are difficult to control.
Periodontal problems associated with orthodontic treatment
A common problem associated with the placement of fixed orthodontic appliances is gingivitis and inflammatory gingival enlargement. It is caused due to inadequate plaque control by the patient. Increased probing depths have been demonstrated in patients with fixed orthodontic appliance with gingival enlargement 121-123. Gingival enlargement can also be seen in patients maintaining good oral hygiene, which is primarily due to the irritation caused by the band or cement 124. The condition improves rapidly within 48 hours after the appliance has been removed.
The orthodontic intrusion of the tooth with non-controlled heavy, intrusive force has been shown to be deleterious as it may result in root resorption, pulp disorders, alveolar bone resorption or an increase in the periodontal bone defects 125. Further, the excessive forces may concentrate at the apical part of periodontal ligament resulting in its hyalinization or necrosis 126. Conflicting results have been found regarding long-term effects of orthodontic treatment on the periodontium. In two retrospective studies 127, 128, no significant adverse effect of orthodontic treatment was found on teeth. On the other hand, another ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
Intrusion changes the relationship between cementoenamel junction and alveolar bone crest. As already stated, tooth intrusion in the absence of adequate plaque control may change dental plaque position from supra-gingival sites to subgingival sites which may result in the formation of infra-bony defects and loss of connective tissue attachment 12.
Investigations have been done to analyze the effect of fixed orthodontic appliances on oral bacteriology. A generalized increase in salivary bacterial counts, especially Lactobacillus, has been demonstrated following placement of orthodontic bands 130. Following the placement of fixed orthodontic appliances, the subgingival microflora has been shown to shift towards periodontopathogenic micro-organisms containing microflora 131. One study 132 investigated changes in the levels of periodontal pathogens before, during and after orthodontic treatment in adolescents. Eight periodontal pathogens were examined including, Aggregatibacter actinomycetemcomitans (AA), Porphyromonas gingivalis (PG), Prevotella intermedia (PI), Tannerella forsythia (TF), Eikenella corrodens (EC), Fusobacterium nucleatum (FN),Treponema denticola (TD), and Campylobacter rectus (CR). The results of the study demonstrated that six (PI, TF, EC, FN, TD, CR) out of eight pathogens were increased following orthodontic treatment. However, the increased levels returned to pre-treatment levels, 12 months after orthodontic treatment. It was concluded that orthodontic treatment with fixed appliance does not increase the risk of increased levels of these periodontal pathogens.
Mucogingival problems associated with orthodontic treatment
The most common mucogingival problem associated with orthodontic treatment is recession. The bodily labial movement of anterior teeth may result in recession if the thickness of gingival tissue and alveolar bone is less. It was observed in one study 133 that labial bodily movement of incisors showed apical displacement of the gingival margin and loss of connective tissue in areas with inflammation. Therefore, if the bodily labial movement of teeth is planned, thin soft tissue and bone, as well as the presence of inflammation, act as risk factors for recession. However, the prevalence of mucogingival defects has been shown to be less (around 5%) in properly treated cases 129. It has been concluded from experimental studies that if the tooth is moved in the envelope of alveolar bone, the risk of side-effects on the marginal soft tissue is minimal 125. The recession has also been observed during tipping movement ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
An adequate width of attached gingiva is a favorable factor for gingival health and it has been shown that a narrow band of attached gingiva is capable of withstanding the stress caused by orthodontic forces 138, 139. It has been suggested that if the minimal width of attached gingiva is present, a free gingival graft should be done to increase the width of attached gingiva before orthodontic treatment is started 140-142.
Another mucogingival problem associated with orthodontic treatment is the appearance of gingival invaginations during space closure. Tooth extraction is a frequently done procedure in orthodontic therapy. First premolars or sometimes second premolars are extracted to create space for tooth movement. The gingival invaginations are superficial changes observed when teeth are moved by orthodontic forces in order to close the space between them. Although, the exact reason for their appearance is unknown, but the break-up of the continuity of the fiber models within the gingiva, and the movement of the root due to orthodontic forces have been suggested as possible reasons 143. In one study, gingival invaginations were observed in around 35% of cases after orthodontic space closure procedures 144. These invaginations may be in the form of slight fissures ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
Periodontally accelerated osteogenic orthodontic (PAOO) treatment
The traditional orthodontic treatment in adults, on an average, takes 18.7 to 31 months more than the adolescent patients 147-149. To reduce the time period of orthodontic treatment, periodontally accelerated osteogenic orthodontic (PAOO) was introduced. To understand PAOO, first, we need to understand the differences between the two terminologies: corticotomy and osteotomy. Corticotomy is defined as a surgical procedure whereby only the cortical bone is cut, perforated, or mechanically altered, without any alterations in the medullary bone. On the other hand, osteotomy refers to the surgical procedure where the cut is given both in the cortical and medullary bone.
Historically, this technique was first described by L C Bryan in 1892 and then Cummingham in 1893 to rapidly correct severe maxillary protrusion with orthodontic appliances 150. The concept of PAOO was further propagated by Heinrick Köle in 1959 with the description of combined radicular corticotomy/supra-apical osteotomy technique 151. The procedure described by Köle included making buccal and lingual interproximal vertical corticotomy cuts, which were extended approximately 1 mm beyond the root apices. These cuts were placed only in the cortical bone. The compartments of bone created in Köle’s technique were referred to as ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
The concept of ‘bony block’ movement prevailed until 2001 when Wilcko et al. (2001) 149 in a study that evaluated the computed tomography scan of patients who had undergone corticotomy, demonstrated that rapid tooth movement was not the result of movement of the bony blocks, but was due to a transient localized demineralization/remineralization process during initial wound healing in the alveolar bony housing which has been referred to as regional acceleratory phenomenon (RAP) 152. The term ‘regional acceleratory phenomenon’ was originally coined by an orthopedist, Harold Frost in 1989 153, 154. He observed that surgical wounding of osseous hard tissue results in striking reorganizing activity adjacent to the site of injury in osseous and/or soft tissue surgery. This increased metabolic activity in bone is a complex physiologic process with dominating features involving accelerated bone turnover and decrease in regional bone densities.
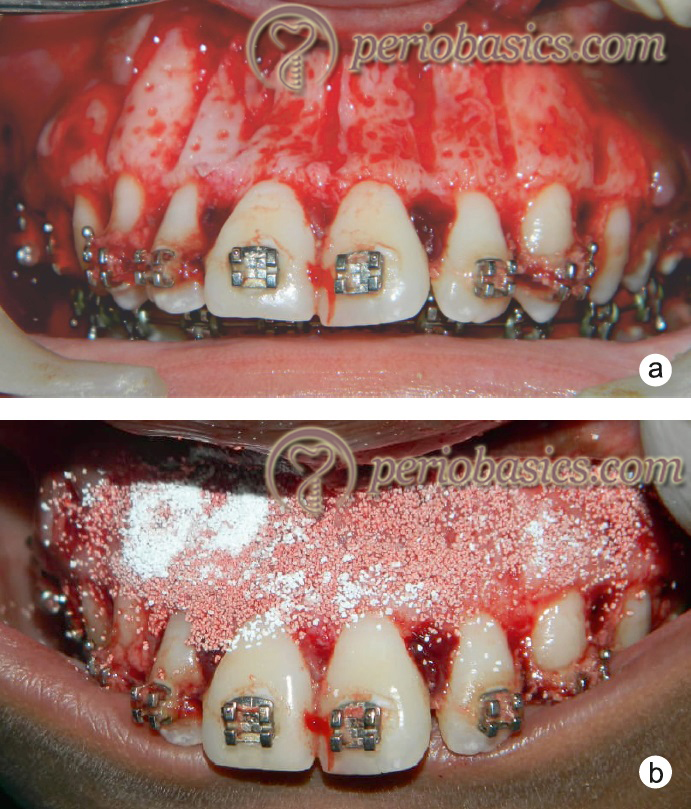
Indications of PAOO treatment:
The major indications of PAOO treatment are,
- Rapidly moving the teeth and reducing the overall treatment time.
- Treatment of moderate to severe malocclusion such as in case of severe bimaxillary protrusion 155.
- Increasing the overall bone volume and avoiding the formation of fenestrations and dehiscences during orthodontic tooth movement.
- Correcting tooth size-arch length discrepancies 156.
- Conservative treatment of class III skeletal discrepancies and avoiding orthognathic surgeries 157-159.
- Cleft-lip and cleft-palate cases 160.
- To accelerate canine retraction after premolar extraction.
- Uprighting of tipped molars and intrusion of supraerupted molars 156, 157.
- To facilitate the eruption of impacted teeth. Surgical traction of impacted teeth, especially the canines, is a frustrating and lengthy procedure. With corticotomy procedure, the traction time is significantly reduced 161, 162.
Clinical procedure:
The clinical procedure of PAOO treatment consists of three steps,
1. Selective alveolar corticotomy,
2. Particulate bone grafting, and
3. Application of orthodontic forces.
Selective alveolar corticotomy:
The first step in the surgical procedure involves selecting the appropriate flap design to perform the corticotomy procedure in the desired areas. The flap should be designed in such a way that it provides complete access to the alveolar bone where corticotomy has to be done. Further, it should be able to fully cover the particulate graft that is placed over the bone surface following corticotomy. The flap should be designed keeping in mind the esthetics as well as the height and shape of interdental papillae. A full-thickness flap is raised in the most coronal aspect of the flap with partial-thickness flap raised near the base of the flap. The advantage of doing so is that partial-thickness flap in the apical area provides flexibility to the flap, hence, improving the adaptability of the flap in its original position after the completion of the procedure. As the procedure involves complete tooth supporting alveolar bone, the horizontal releasing incision should be extended sufficiently distal to avoid the need for the ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
Once the flap has been raised, vertical corticotomy cuts are made in the interdental areas with round burs with saline irrigation. The vertical cuts are extended approximately 2 mm beyond the root apices and are connected with horizontal corticotomy cuts. At the coronal end, the vertical cuts should stop approximately 2 mm short of the alveolar crest. If the alveolar bone has sufficient thickness, solitary perforations may be placed in the alveolar bone over the radicular surface. However, if it is anticipated that alveolar bone thickness is less than 1-2 mm, the perforations in the cortical one are not done to prevent any damage to the root surface. Another modification of the corticotomy technique includes placement of triangular corticotomy cuts, which are specifically indicated in cases of too thin buccal cortical bone.
Particulate bone grafting:
Particulate bone graft placement has been advocated in corticotomy procedures to increase the bone volume in the operated area. The grafting may be done with various bone grafts such as bovine xenografts, decalcified freeze-dried bone allografts, autogenous bone grafts and combination of these. Most commonly the quantity of the graft used ranges between 0.25 to 0.5 mL per tooth 156. However, the amount of bone graft used may vary according to the pre-existing alveolar deficiencies. It must be kept in mind that a ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ………. Contents available in the book ……….
After the placement of the bone graft, the mucoperiosteal flap is sutured back in its original position. If the recession is present in the operated area, the flap can be coronally advanced or connective tissue graft may be used to cover the recession. The patient is put on antibiotics and analgesics for infection and pain control respectively. It should be noted that analgesics should not be continued beyond one week post-operatively. This is because these can inhibit the natural inflammatory process that is required for rapid tooth movement.
Application of orthodontic forces:
The last step of the procedure is the application of appropriate orthodontic forces on the teeth. Post surgically, immediate heavy orthodontic forces should be applied on the teeth. This is because we have limited time to achieve accelerated tooth movement. The initiation of orthodontic forces should not be delayed for more than 2 weeks.
Conclusion
There is a universal consensus regarding maintenance of good oral hygiene during orthodontic treatment. The most important factors determining the overall success of orthodontic treatment in a periodontally compromised patient are proper diagnosis before initiation of orthodontic therapy and continued observation of periodontal condition throughout the active orthodontic treatment. Along with this, a continued dialogue should be maintained with the patient to reinforce the maintenance of good oral hygiene. The orthodontist treating the case must have an in-depth knowledge of tooth movement in different types of bone defects and tooth movement should be planned in such a way that the overall periodontal support of tooth is increased after the treatment. On the other hand, it is the duty of the periodontist to identify the types of bone defects and do the needful treatment before the orthodontic treatment is initiated. It should be remembered that in a periodontally compromised case, the overall success of the orthodontic treatment depends on the combined effort and close monitoring of the case, both by an orthodontist and a periodontist. Hence, these cases need special attention and should be carefully planned and treated.
References
References are available in the hard-copy of the website.
Periobasics: A Textbook of Periodontics and Implantology
The book is usually delivered within one week anywhere in India and within three weeks anywhere throughout the world.

