Introduction to clinical features of normal gingiva
The knowledge regarding the normal features of the gingiva is essential to understand the pathological changes that occur in the periodontium in various periodontal diseases. Periodontitis is an inflammatory disease with microbial etiology being its primary etiology. There are various inflammatory changes that can be seen in periodontitis. To understand the histopathological changes that occur in these inflammatory conditions, first, we should know the normal physiology of the periodontium. Various clinical features of normal gingiva can be co-related to the microscopic findings. These are,
Color
The color of the normal gingiva is pale or coral pink. There are four factors that determine the color of the gingiva. These are vascular supply, the thickness of the epithelium, the degree of keratinization and physiologic pigmentation. During chronic inflammation, the gingiva may appear reddish pink/bluish in color, whereas during acute inflammation it may appear bright red in color. These changes during inflammation are because of increased blood flow, increased permeability of capillaries, and increased collection of defense cells and tissue fluid. The color of healthy gingiva is different from the alveolar mucosa which is red in color. Also, the alveolar mucosa is smooth and shiny rather than stippled as seen in the attached gingiva.

The thickness of the epithelium also affects the color of the gingiva. It varies from individual to individual. As discussed earlier, there are two types of periodontal phenotypes: thin and thick. Pigmentation in gingiva is produced by melanin-producing cells, the melanocytes. The melanin pigmentation of the gingiva varies with race and complexion. It is lighter in blond individuals with a fair complexion as compared to the dark-complexioned individuals. The gingival pigmentation is minimal in Caucasian individuals, whereas African and Asian individuals have brown or bluish-black areas of pigmentation.
Surface texture
As already stated, the surface of the attached gingiva is stippled, demonstrating an ‘orange peel appearance’. Stippling is present on the attached gingiva and interdental papillae. It should be viewed after drying the gingiva with cotton, under broad daylight and not under the dental chair light. This is because dental chair light is focused, whereas the broad daylight comes from all directions, thus making stippling more visible. It is usually absent in children less than 5 years of age and in elderly individuals. It is more prominent on the labial surface as compared to the lingual surface and may be absent in some individuals.
Histologically, stippling corresponds to the epithelial and connective tissue inter-digitations. The rete ridges and rete peg arrangement between the connective tissue and the epithelium in the gingiva provides excellent stability to the attached gingiva to withstand mechanical forces. The degree of keratinization also determines the surface texture of the gingiva. Both stippling and epithelial keratinization are adaptive responses to mechanical forces during mastication, speech, and deglutition. However, it must be remembered that the epithelial keratinization is genetically determined. Connective tissue carries the genetic information about the overlying epithelium. In free gingival grafts, when connective tissue is transplanted from the keratinized to the nonkeratinized site, it becomes covered by keratinized epithelium 201.
Contour
The normal contour of the gingiva is scalloped with knife-edge gingival margins. The attached gingiva has a festooned appearance with intermittent prominences corresponding to the root surface contour. The contour of the gingiva depends on the shape and alignment of the teeth in the dental arch. When teeth are more labially placed, the contour of the gingiva becomes accentuated and when teeth are more lingually placed, the contour of the gingiva becomes more horizontally flattened. Along with this, the position and size of the contact area and dimensions of the embrasures also determine the gingival contour.

Shape
The shape of the interdental papilla is determined by the location and shape of the interproximal contact and contour of the proximal tooth surfaces. In anterior teeth, the interdental papilla is pyramidal-shaped, whereas, in the posterior teeth, it is flat or saddle-shaped.
Size
The size of the gingiva refers to the sum total of the cellular and connective tissue components of the gingiva. Change in the size of gingiva is associated with pathological conditions. For example, in the case of gingival enlargement, the connective tissue component of the gingiva is increased.
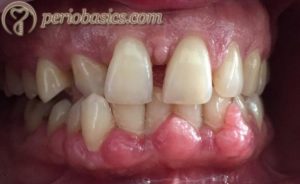
Consistency
The consistency of the normal gingiva is firm and resilient. The gingiva is palpated with a blunt instrument to check for its consistency. The gingival connective tissue is composed of collagen fibers and is firmly bound to the underlying mucoperiosteum, giving it a firm and resilient consistency. During gingival inflammation, the gingival consistency becomes soft and edematous. This is because of the increased vascular flow, increased vascular permeability, and fluid accumulation.
Conclusion
In the above discussion, we discussed various normal features of the gingiva. An in-depth understanding regarding these features is essential to understand the pathological changes that occur in various diseases of the periodontium.
References
References are available in the hard copy of the website.
Periobasics A Textbook of Periodontics and Implantology
The book is usually delivered within one week anywhere in India and within three weeks anywhere throughout the world.

