Introduction to immunity
Immunity is defined as resistance to disease, specifically infectious disease. The immune system is the collection of cells, tissues, and molecules that functions to defend us against infectious microbes. The main function of the immune system is to prevent or limit infections. This defense function of the immune system is essential for our ability to survive in an environment that has potentially deadly microbes. But, immune responses can also be damaging. Many autoimmune diseases are caused by uncontrolled or excessive immune responses against self-antigens (e.g. rheumatic fever, asthma, glomerulonephritis, many dermatological disorders, and multiple sclerosis, etc.)
Immunity can be classified as:
- Innate (with which individual is born)
- Acquired (which person acquires)
Immunity has mainly two components:
- Cell-mediated immunity.
- Antibody-mediated immunity.
Two other major components are:
- Complement system.
- Phagocytic system.
Before we study the Cell-mediated immunity (CMI) and Antibody-mediated immunity (AMI), here is a brief description of the lymphoid system,
Lymphoid system
The body uses the lymphoid system to enable lymphocytes to encounter antigens and it is here that adaptive immune responses are initiated. The organs involved in specific as well as non-specific immunity are classified as primary (central) lymphoid organs and secondary (peripheral) lymphoid organs. The blood and lymphatic vessels that carry lymphocytes to and from the other structures can also be considered lymphoid organs.
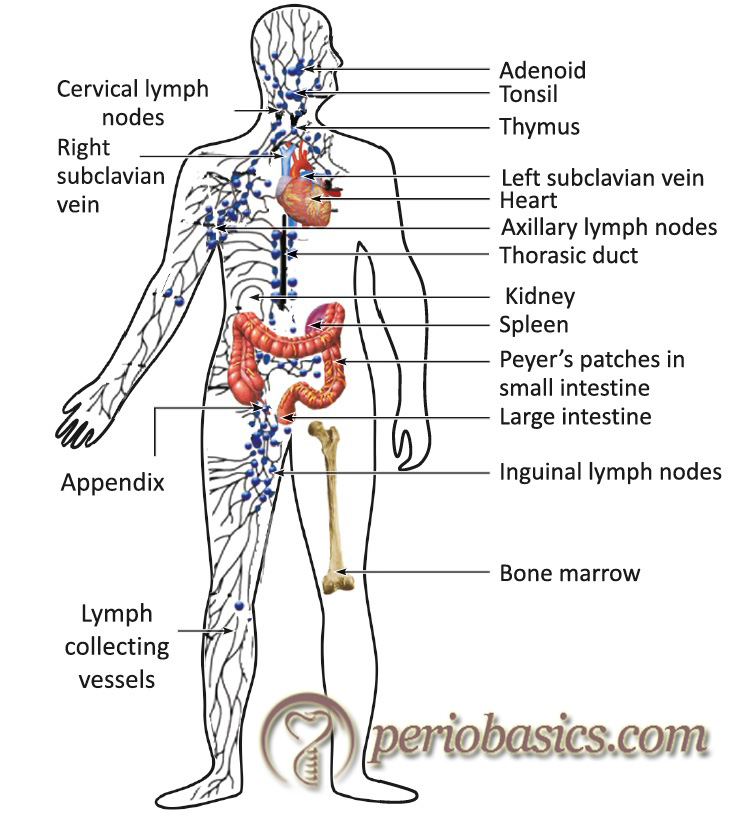
Primary lymphoid organs
These are sites of antigen-independent lymphocyte proliferation. Here B and T lymphocytes differentiate from lymphoid stem cells into mature albeit naïve effector cells. These include the following:
- Bone marrow.
- Thymus
Secondary or peripheral lymphoid organs
Secondary lymphoid organs provide an environment that enables lymphocytes to interact with each other, with accessory cells, and with antigens, resulting in the initiation of antigen-specific primary immune responses.
- Lymph node.
- Spleen.
- Peyer’s patches.
- Tonsils.
- Adenoids.
- Appendix.
- Mucosa-associated lymphoid tissue (MALT).
Here is a brief description of these lymphoid organs:
Bone marrow:
Bone marrow is the primary source of all the cells of the immune system. During fetal development, hematopoiesis occurs initially in the yolk sac and para-aortic mesenchyme and later in the liver and spleen. Then it gradually shifts to bone marrow. The bone marrow is the site of origin of all T- and B- cells, mononuclear phagocytes, platelets, erythrocytes, and other leukocytes in the adult. The bone marrow is divided into wedge-shaped hematopoietic compartments filled with proliferating and differentiating blood cells in connective tissue matrices bordered by venous sinuses.
Thymus:
This lymphoepithelial organ develops from ectoderm derived from the third branchial cleft and endoderm of the third branchial pouch including mesenchymal components derived from cells of the cephalic neural crest which all migrate from the neck to the anterior mediastinum. It reaches its greatest size just prior to birth, then atrophies with age. The major function of the thymus is …………. Contents available in the book…………. Contents available in the book…………. Contents available in the book…………. Contents available in the book….
Periobasics: A Textbook of Periodontics and Implantology
The book is usually delivered within one week anywhere in India and within three weeks anywhere throughout the world.
India Users:
International Users:
Lymph nodes:
There are numerous lymph nodes disseminated all over the body. They measure 1–25 mm in diameter and play a very important and dynamic role in the initial or inductive states of the immune response.
Anatomical structure of lymph node: The lymph nodes are circumscribed by a connective tissue capsule. They receive afferent lymphatics draining peripheral interstitial spaces and also receive blood from the systemic circulation through the hilar arteriole. Lymph node has two main regions: the cortex and the medulla. The cortex and the deep cortex (also known as paracortical area) are densely populated by lymphocytes, in constant traffic between the lymphatic and systemic circulation. In the cortex, at low magnification, one can distinguish roughly spherical areas containing densely packed lymphocytes, termed follicles or nodules.
It is important to note that T and B-lymphocytes occupy different areas in the cortex. B-lymphocytes predominate in the follicles (hence, the follicles are designated as T-independent area), which also contain macrophages, follicular dendritic cells, and some T lymphocytes.
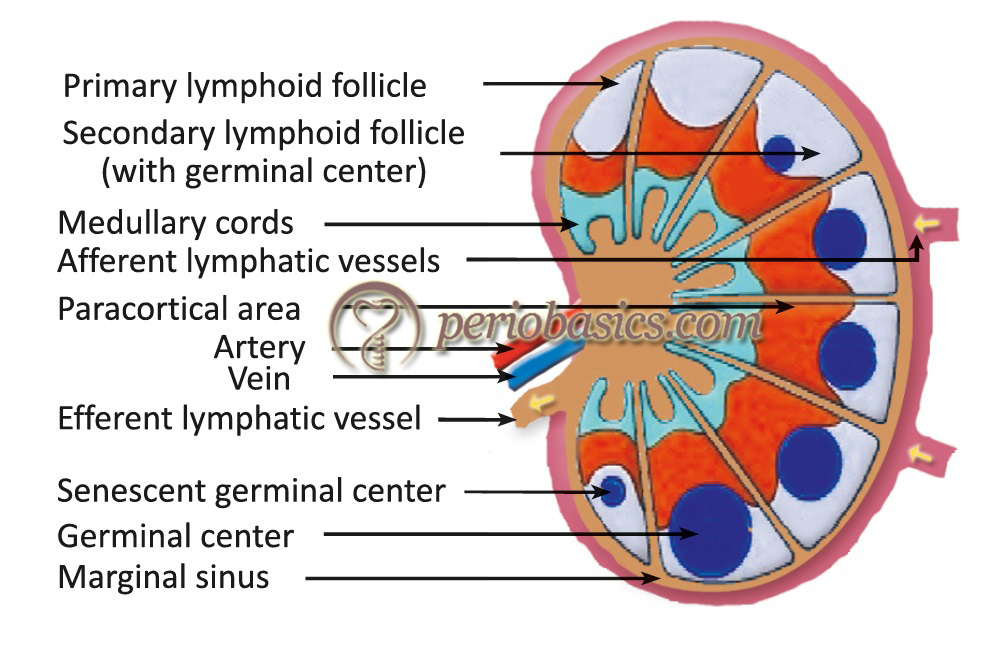
Spleen:
Weighing about 150 grams, the spleen is the largest single lymphoid organ in the body. It is situated in the left upper quadrant of the abdomen. It is covered by dense fibrous capsule with muscular trabeculae extending inward to subdivide the spleen into lobules. Its major functions are filtration of blood and it is the major organ in which antibodies are synthesized and released into circulation. Patients with splenectomy (removal of the spleen) are highly susceptible to infections with capsulated bacteria such as pneumococci and meningococci.
Mucosa-associated lymphoid tissue (MALT):
“MALT” refers to a diffuse collection of lymphoid tissues that line the respiratory, alimentary, and genitourinary tracts. MALT produces the immune responses against pathogens that invade the mucosa that lines these tracts. Like the spleen and lymph nodes, the MALT contains B-cell follicles and distinct T-cell-rich regions. In the intestine, we find Peyer’s Patches and the tonsils are similar structures in the upper alimentary tract. Although its organization is similar to the spleen and lymph node, the mucosal immune system is different in several ways: (1) unlike the spleen and lymph node, MALT tissue is not surrounded by a fibrous capsule, (2) IgA is the predominant class of immunoglobulin produced in MALT (3) It is not filtering Ag delivered by vessels like the blood vessels or lymphatic vessels.
Know More…
Lymphatic circulation:
Blood circulating through the body leaks into tissues through the thin walls of the capillaries. This portion of blood plasma that escapes is called interstitial fluid. Lymphatic capillaries reabsorb the excessive tissue fluid and transport the fluid through the lymphatic pathway, and ultimately dispose it into the blood. When this extracellular fluid enters the lymphatic system it is called lymph. It drains into larger vessels called the lymphatics. These vessels converge to form one of two large vessels called lymphatic trunks, which are connected to veins at the base of the neck. One of these trunks, the right lymphatic duct, drains the upper right portion of the body, returning lymph to the bloodstream via the right subclavian vein. The other trunk, the thoracic duct, drains the rest of the body into the left subclavian vein. The lymphatic pathway is an open circuit where lymphatic capillaries in body tissues reabsorb excessive tissue fluid which is derived from blood plasma. This lymph ultimately returns to the blood plasma (i.e. blood plasma in capillaries → interstitial fluid → lymph in the lymphatic pathway →lymph returns to blood plasma).
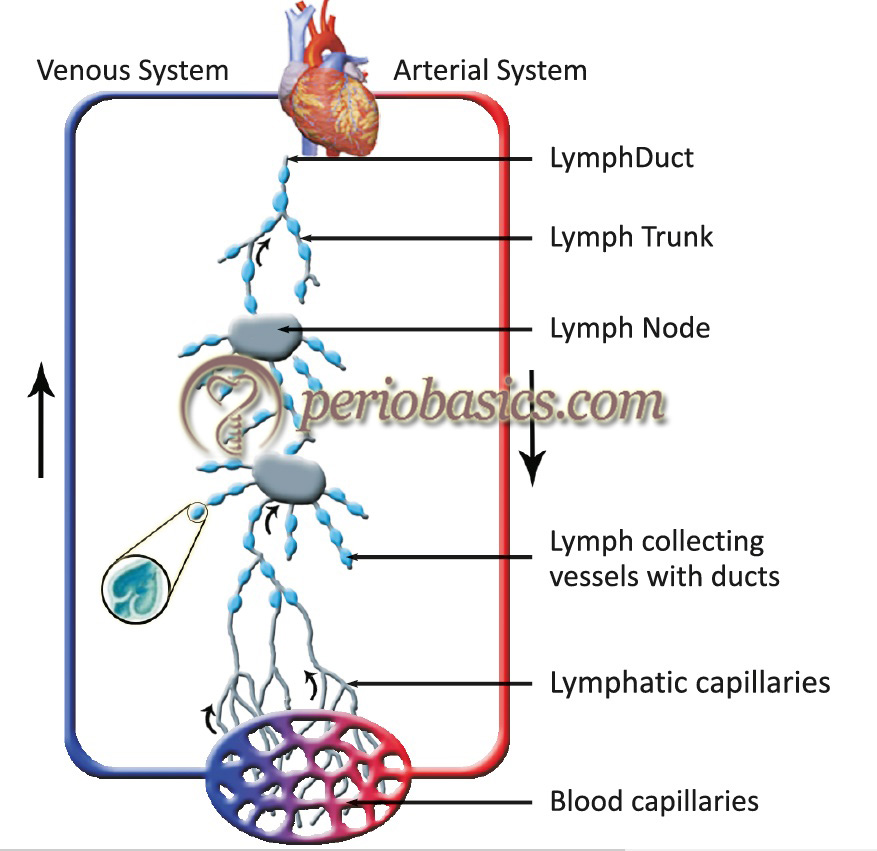
Cell-mediated and antibody-mediated immunity
Cell-mediated immunity (CMI) consists of T Lymphocytes- helper and cytotoxic T-cells. Antibody-mediated immunity (AMI) consists of B lymphocytes and plasma cells. Cell-mediated immunity provides defense against tuberculosis, viruses and fungi, allergy (poison oak), graft rejection and helps in regulation of antibody response. Antibody-mediated immunity provides defense against bacterias by opsonization, neutralization of toxins and viruses, hay fever and is a cause of autoimmunity. So the main function of antibody-mediated immunity is neutralization and opsonization, and the main function of cell-mediated immunity is inhibition of organisms kills certain intracellular bacteria and tumor cells.
Common features of CMI and AMI:
- Diversity (respond to millions of antigens),
- Memory (Memory T- and B-cells), and
- Specificity (action is directed against a particular).
Helper T-cells and macrophages mainly provide intracellular immunity whereas the cytotoxic T-cells destroy the virus-infected cells. Humoral immunity is our basic defense against extracellular encapsulated bacteria such as staphylococcus and streptococcus etc. Antibodies neutralize toxins.
Innate immunity
Innate immunity, which is the first line of defense against invasion by microbes. Refers to any inborn resistance that is present the first time a pathogen is encountered; it does not require prior exposure and is not modified significantly by repeated exposures to the pathogens over the life of an individual. The responses include inflammation, phagocytosis by leukocytes, natural killer cells, tissue secretion, and complement. It can be,
- Extrinsic
- Intrinsic
Extrinsic: provided by Skin, mucous membrane, cough reflex, chemical influences like fatty acids and pH.
Intrinsic: Fever inhibits the growth of micro-organisms, interferons and other substances released by leukocytes; serum proteins (beta-lysin, lysozyme, polyamines, and kinins) counter the microorganisms. Other phagocytic cells, granulocytes, macrophages, and macroglial cells also provide innate immunity.
Know More…
Role of Macrophages in innate immunity:
These are derived from monocytes present in the blood. These migrate to different tissues to form a variety of specialized histological forms called the reticuloendothelial system (RES). They trap the foreign body and sed RBC’s . Macrophages produce several cytokinins. Most important of these are IL-1 (activation of CD-4) and TNF (mediator of inflammation). They differentiate into different varieties and forms:
1) Kuffer’s cells in the liver
2) Alveolar macrophages in lungs
3) Splenic macrophages in the white pulp
4) Peritoneal macrophages freely floating in peritoneal fluid
5) Macroglial cells in CNS
Macrophages have two major functions:
1) To engulf foreign particles, and with the help of enzymes, its break down.
2) To take up the, process them by denaturation or by partial digestion and present them on the surface of specific T-cells. Thus, function as presenting cells (APCs). The cells belonging to APCs include dendritic cells of spleen and lymph nodes, interdigitating cells of the thymus, Langerhans cells of the skin etc.
These are not potent phagocytotic but are potent APCs. So, monocytes play a key role in immunity. As they participate both in innate the acquired immunity response, they are component of both innate and acquired immunity.
Acquired immunity
It is also called specific or acquired immunity. It is more specialized than innate immunity and it supplements the protection provided by innate immunity. It is the type of host defense that is stimulated by microbes that invade tissues, that is, it adapts to the presence of microbial invaders. It is an evolutionary immunity and is present only in the vertebrates. It is acquired by contact with the invader and is active against only that invader. Edward Jenner in 18th century experimentally induced immunity to smallpox (he introduced young boy with pus from a lesion on dairymaid who had cowpox and then introduced with smallpox virus). The term vaccine is derived from the Latin word (Vacca– cow) in this way.
Types of acquired immunity
- Active: immunization by giving antigen.
- Passive: transfer of antibodies from immunized individual to non-immunized individual.
- Adoptive: transfer of immunity by transfer of immune cells.
Characteristics of the immune response:
- Specificity.
- Adaptiveness.
- Discrimination between self and non-self (done by specialized cells i.e, lymphocytes).
- Memory.
Cells involved in the acquired immune response
T-cells, B-cells and APCs are involved in the acquired immune response. Humoral immunity is mediated by proteins called antibodies, which are produced by cells called B-lymphocytes. Antibodies are secreted into the circulation and mucosal fluids, and they neutralize and eliminate microbes and microbial toxins that are present outside of host cells, in the blood and in the lumens of mucosal organs, such as the gastrointestinal and respiratory tracts. T-lymphocytes (which mature in the thymus) function mainly to combat microbes that have learned to live inside cells (where they are inaccessible to antibodies). T-cells can be broadly divided into both T-helper (Th) and cytotoxic T-cells (Tc). Furthermore, Th cells may be sub-divided into …………. Contents available in the book…………. Contents available in the book…………. Contents available in the book…………. Contents available in the book……
Periobasics: A Textbook of Periodontics and Implantology
The book is usually delivered within one week anywhere in India and within three weeks anywhere throughout the world.
India Users:
International Users:
Mechanism of generation of the humoral immune response
When antigens enter the connective tissue after crossing the epithelial barrier or enter the bloodstream, they are first concentrated in the lymph nodes, spleen, and other lymphoid tissues. Here the antigens are recognized by the small number of B-cells that express specific receptors for the antigens. These B-cells then become activated and they undergo two important changes. First, the B-cells divide, leading to an increase in the number of -specific cells and second, the B-cells start producing more antibody and secreting this antibody, so that it can circulate freely and counter the antigens. Antibody secreting cells, called plasma cells, are the effector cells of the B lymphocyte lineage. If the antigen is a protein, it also activates helper T-cells. These helper T-cells interact with the -specific B-cells and enhance antibody secretion; in fact, helper T-cells are absolutely required for effective antibody responses against protein antigens. Also, helper T-cells stimulate the B cells to secrete different classes of antibodies (also called isotypes).
Mechanism of generation of the T-cell response
T-Lymphocytes are the cells involved in cell-mediated immunity. The T-cell receptors of most T-lymphocytes only recognize peptide fragments of protein s that are bound to specialized peptide display molecules called major histocompatibility complex (MHC) molecules, on the surface of specialized cells called -presenting cells (APCs). For a detailed description of MHC please read ‘Major histocompatibility complex’ and for T-cells and MHC molecule interactions please read ‘Interactions between antigen-presenting cells and T-cells’ in the other section of the website.
Tumor Immunity
In animal studies, it has been shown that they develop resistance to the chemically or virally induced tumors. This is because during tumor formation new antigens called tumor-associated antigens (TAA) develop on the surface of cells that are recognized as foreign or ‘non-self’. Chemically induced tumors have TAA’s which are specific for a particular tumor and differ from other tumors. Virally induced TAA’s are non-specific for a tumor and cross-react with two or more tumors induced by the same virus. TAA’s induce on the cell surface by different viral cells do not cross-react. Immune surveillance detects the newly arising clones of malignant cells. This immune response is weak and can be overcome by a large dose of tumor cells. Tumor cells can escape surveillance by modulation i.e. Internalization of the surface antigen’s so that they no longer present to immune attack. The immune response against tumor include,
- NK cells- which act without antibodies.
- Killer cells which mediate antibody-dependent cytolysis
- Cytotoxic (CD8)T-cells
- Activated macrophages.
Two types of antibodies are produced against tumor antigens; cytotoxic and blocking antibodies. The blocking antibodies induce tumor growth as these hinder the reorganization of tumor antigen by antibodies. One interferon TNF-α is found effective against many solid tumors. In addition lymphocytes activated by IL-2(Lymphokines activated cells)i.e. LAK cells are useful in cancer immunotherapy.
TIL-Tumor infiltrating lymphocytes
Another cancer immunotherapy involves the use of TIL- tumor-infiltrating lymphocytes. The basis of this therapy is that some cancers are infiltrated by NK-cells and cytotoxic T-cells that seem to destroy tumor cells. The lymphocytes are surgically removed cancer and grown in cultures until a large number of cells are produced activated with IL-2. These are then injected in the same patient.
Some tumors contain Antigen’s that normally occur in fetal but not in adult cells
- Carcinoembryonic antigen: It is elevated in the serum of patients with carcinoma colon, pancreas, breast & liver. It is found in the gut, liver, pancreas or fetus in small quantities. This antigen is not helpful in diagnosis but it is helpful in the management of tumors. If it’s level decline after surgery, it means that the tumor is not spreading but elevated suggest recurrence.
- α-Fetoprotein: Elevated in patients of hepatoma. It is found in fetal liver and can rise in many other specific malignant or non-malignant diseases.
Conclusion
We are living in an environment that is full of some deadly micro-organisms. For thousands of years, humans and these organisms have been surviving and living with each other. The primary reason for our survival is a highly efficient immune system that is able to identify almost every microorganism that enters our body. An immune response that may be antibody-mediated or antigen mediated is generated against that microorganism that eliminate the infection from the body. If our immune system is not able to identify and eliminate the microorganisms, it may result in the death of the individual. Thus, the understanding of the immune system is very important to know the host microbial interactions.

